What Exactly Is Posterior Tibial Tendon Dysfunction ?
Overview
Adult flatfoot may be due to multiple problems including a dysfunctional posterior tibial tendon (PTT), hypermobility and ligamentous laxity, or possibly a coalition that becomes symptomatic. For a vast majority of patients, posterior tibial tendon dysfunction (PTTD) is the cause of symptomatic flatfoot and is the main trigger of surgical reconstruction in flatfoot. The common presenting scenario for adult flatfoot is a case of unilateral flatfoot with pain. Patients will often confirm they ?always had flat feet? but have noticed increased pain and additional collapse in the past few months to years. They may also note increased swelling and a possible concern over one foot increasing in shoe size. After a comprehensive dermatologic, neurologic and vascular assessment, one should direct his or her attention to the musculoskeletal portion of the exam. It is key to examine the foot and leg as a whole in order to determine the proper procedure and consider each phase of the corrective surgery. 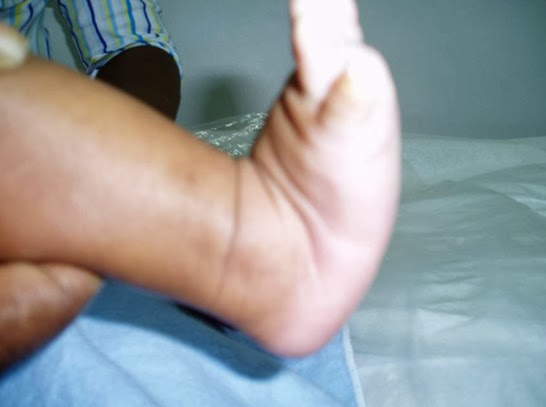
Causes
Rheumatoid arthritis This type of arthritis attacks the cartilage in the foot, leading to pain and flat feet. It is caused by auto-immune disease, where the body?s immune system attacks its own tissues. Diabetes. Having diabetes can cause nerve damage and affect the feeling in your feet and cause arch collapse. Bones can also fracture but some patients may not feel any pain due to the nerve damage. Obesity and/or hypertension (high blood pressure) This increases your risk of tendon damage and resulting flat foot.
Symptoms
Often, this condition is only present in one foot, but it can affect both. Adult acquired flatfoot symptoms vary, but can swelling of the foot's inner side and aching heel and arch pain. Some patients experience no pain, but others may experience severe pain. Symptoms may increase during long periods of standing, resulting in fatigue. Symptoms may change over time as the condition worsens. The pain may move to the foot's outer side, and some patients may develop arthritis in the ankle and foot.
Diagnosis
Posterior Tibial Tendon Dysfunction is diagnosed with careful clinical observation of the patient?s gait (walking), range of motion testing for the foot and ankle joints, and diagnostic imaging. People with flatfoot deformity walk with the heel angled outward, also called over-pronation. Although it is normal for the arch to impact the ground for shock absorption, people with PTTD have an arch that fully collapses to the ground and does not reform an arch during the entire gait period. After evaluating the ambulation pattern, the foot and ankle range of motion should be tested. Usually the affected foot will have decreased motion to the ankle joint and the hindfoot. Muscle strength may also be weaker as well. An easy test to perform for PTTD is the single heel raise where the patient is asked to raise up on the ball of his or her effected foot. A normal foot type can lift up on the toes without pain and the heel will invert slightly once the person has fully raised the heel up during the test. In early phases of PTTD the patient may be able to lift up the heel but the heel will not invert. An elongated or torn posterior tibial tendon, which is a mid to late finding of PTTD, will prohibit the patient from fully rising up on the heel and will cause intense pain to the arch. Finally diagnostic imaging, although used alone cannot diagnose PTTD, can provide additional information for an accurate diagnosis of flatfoot deformity. Xrays of the foot can show the practitioner important angular relationships of the hindfoot and forefoot which help diagnose flatfoot deformity. Most of the time, an MRI is not needed to diagnose PTTD but is a tool that should be considered in advanced cases of flatfoot deformity. If a partial tear of the posterior tibial tendon is of concern, then an MRI can show the anatomic location of the tear and the extensiveness of the injury.
Non surgical Treatment
Stage one deformities usually respond to conservative or non-surgical therapy such as anti-inflammatory medication, casting, functional orthotics or a foot ankle orthosis called a Richie Brace. If these modalities are unsuccessful surgery is warranted. 
Surgical Treatment
Surgical treatment should be considered when all other conservative treatment has failed. Surgery options for flatfoot reconstruction depend on the severity of the flatfoot. Surgery for a flexible flatfoot deformity (flatfoot without arthritis to the foot joints) involves advancing the posterior tibial tendon under the arch to provide more support and decrease elongation of the tendon as well as addressing the hindfoot eversion with a osteotomy to the calcaneus (surgical cut in the heel bone). Additionally, the Achilles tendon may need to be lengthened because of the compensatory contracture of the Achilles tendon with flatfoot deformity. Flatfoot deformity with arthritic changes to the foot is considered a rigid flatfoot. Correction of a rigid flatfoot deformity usually involves surgical fusion of the hindfoot joints. This is a reconstructive procedure which allows the surgeon to re-position the foot into a normal position. Although the procedure should be considered for advanced PTTD, it has many complications and should be discussed at length with your doctor.